I was reviewing spirometry reports and noticed several patients in a row with an early termination of exhalation that was not reflected in the reported expiratory time. This is far from the first time I’ve noticed this but seeing several examples more or less at the same time got me curious about how the software was determining expiratory time.
The ATS/ERS standards are somewhat mute on how the total expiratory time of a spirometry effort is determined. The closest the standard comes to addressing this is the end-of-test (EOT) criteria:
“The volume–time curve shows no change in volume (<0.025 L) for >=1 s[econd]”
But this is meant primarily as a quality indicator to show the patient has really achieved an adequate exhalation and not as a definition of expiratory time. In fact total expiratory time is not defined in the ATS/ERS standards at all and this leaves it up to individual equipment manufacturers to determine when a spirometry effort is over. This is a problem because the ATS/ERS standards also say that patients should:
“exhale for >=3 s in children aged <10 yrs and for >=6 s in subjects aged >10 yrs.”
So despite not being defined, the length of a spirometry effort is a critical quality indicator.
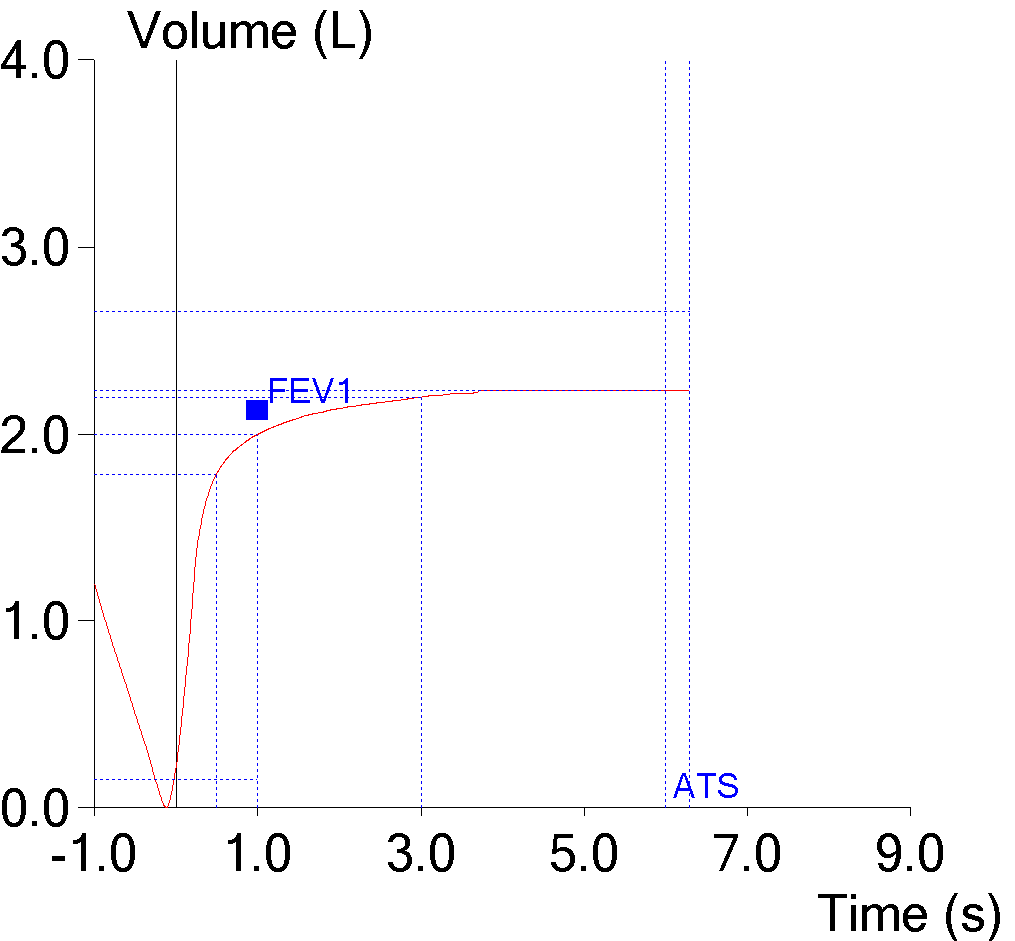
This spirometry effort was reported at being 6.41 seconds long, but it is clear the patient stopped exhaling well before that time. I downloaded the raw data for the effort into a spreadsheet and by looking at the volume and flow results I was able to see the patient had actually exhaled for 3.96 seconds. During the final 2.45 seconds there was no change in volume (the maximum change was 0.007 L, which is probably due to electronic noise). This makes it apparent that even if there is no change in expiratory volume our spirometry software continues to time the effort.