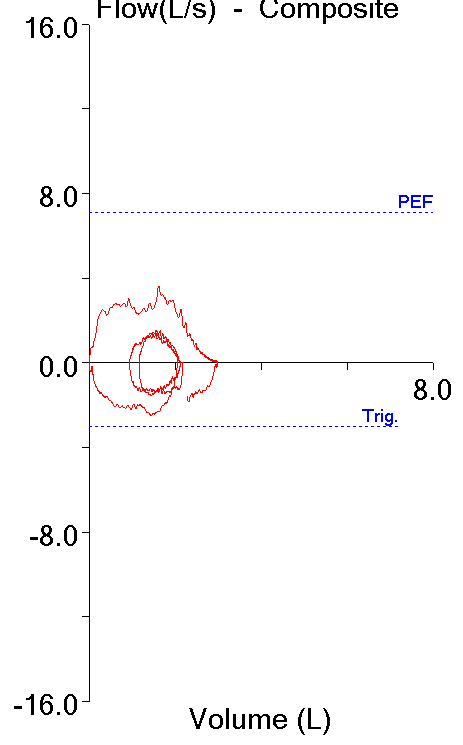
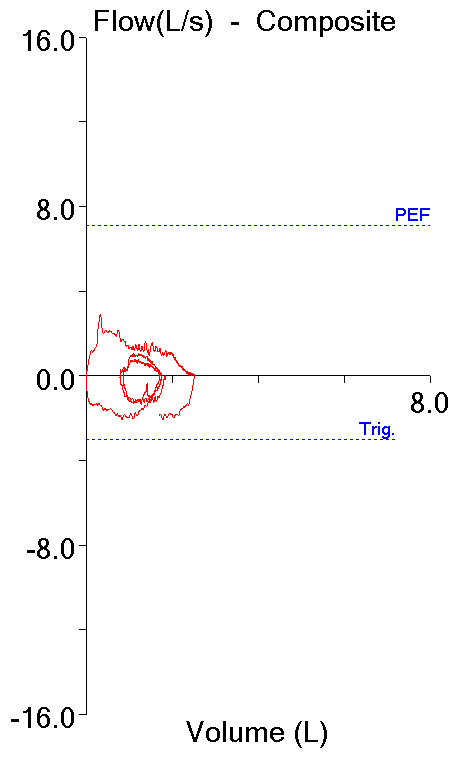
Recently I was reviewing a spirometry report and noticed that the FVC was below normal. A low FVC can suggest a restrictive lung disease but the reported expiratory time was only about 4 seconds. I took a look at the graphics included with the report and the volume-time curve showed the effort ended well before 6 seconds so my first thought was that the reduced FVC was more likely because of suboptimal patient effort than anything else.
I always try to review spirometry results whenever there is anything questionable so I pulled up the raw test results and immediately saw that the reported FVC was actually a composite. The ATS-ERS statements on Spirometry and Interpretation say that the highest VC regardless of which test it came from (which even includes the slow vital capacity test from lung volume measurements and the inspiratory volume from a DLCO) should be used when reporting spirometry results. In this case the FVC came from one effort, the FEV1 and everything else came from a different effort. The interesting thing was that the effort the FVC came from was about 10 seconds long which shows it actually was an adequate effort. The FEV1 effort on the other hand was only about 4 seconds long and showed an abrupt and early termination of exhalation.
The technician who performed the tests selected the correct efforts to make a composite. The patient had made five spirometry efforts and the selected FVC was significantly larger than all of the other efforts but the FEV1 from the same effort was significantly lower than several other efforts. Our criteria for selecting FEV1 does not just go by the largest FEV1, we also look at the peak flow (PEF) and whether there has been any back extrapolation and the effort the FEV1 came from had the highest peak flow and no back extrapolation. So, a good choice had been made on both efforts.
When it comes to selecting values from different spirometry efforts there are only a limited number of results that our lab software allows us to mix and match. The FVC, the FEV1 and the graphics (flow-volume loop and volume-time curve which are linked to each other) can all be selected individually, but everything else, which includes the expiratory time, PEF, FEF25-75, MEF50 etc. etc. can only be selected as a group.
Continue reading →