I would like to re-emphasize the importance of the descriptive part of CPET interpretation. At the very least consider it to be a checklist that should always be reviewed even when you think you know what the final interpretation is going to be.
After gas exchange, the next step in the flow of gases is circulation. The descriptive elements for assessing circulation are:
What was the maximum heart rate?
The maximum predicted heart rate is calculated from 220 – age.
A maximum heart rate above 85% of predicted indicates that there has been an adequate exercise test effort.
Example: The maximum heart rate was XX% of predicted {which indicates an adequate test effort}.
What was the heart rate reserve?
The heart rate reserve is (predicted heart rate – maximum heart rate). A heart rate reserve that is greater than 20% of the (predicted heart rate – resting heart rate) is elevated and may be an indication of either chronotropic incompetence or an inadequate test effort.
Note: A negative heart rate reserve will occur whenever a patient exceeds their predicted heart rate.
Example: The heart rate reserve is XX BPM which is {within normal limits | elevated}.
What was the heart rate recovery (HRR)?
The heart rate recovery is the (maximum heart rate – heart rate at 1 minute post-exercise). A HRR < 12 indicates the patient has a reduced vagal and parasympathetic tone and carries a higher mortality risk.
Example: The heart rate recovery was XX BPM which is {within normal limits | reduced}.
What was the chronotropic index?
The chronotropic index relates the change in heart rate to the change in oxygen consumption. A chronotropic index > 1.30 indicates a steep heart rate response and can suggest an increased dependence on heart rate to increase cardiac output secondary to a low stroke volume. A chronotropic index < 0.8 can indicate a blunted heart rate response (possible chronotropic incompetence) which in turn can suggest a variety of cardiac dysfunctions but can also be caused by medication (beta blockers). A low chronotropic index can also be seen in exceptionally fit individuals (elevated max VO2, elevated VO2 at AT), and in these cases, is normal. In an exceptionally fit individual a normal chronotropic index is likely abnormal.
Note: Chronotropic index is calculated from:
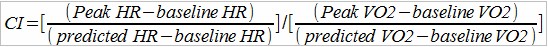
and is discussed in greater detail in the previous posting Chronotropic Index and O2 Pulse.
Example: The Chronotropic Index was X.XX which is {reduced | within normal limits | elevated|.
What was the resting and maximum exercise blood pressure?
A normal max systolic pressure during exercise is 160-220 mm Hg. A normal increase in diastolic pressure during exercise is 10 mm Hg. A diastolic pressure during exercise greater than 90 Hg is likely abnormal and greater than 100 mm Hg is definitely abnormal and suggests diastolic dysfunction. If systolic blood pressure did not increase to greater than 130 mm Hg, or dropped >10 mm Hg during exercise, consider left ventricular dysfunction, possible CAD
Note: Guidelines for the maximum allowable blood pressure during exercise remain unclear. We use a diastolic pressure ≧ 110 mm Hg or a systolic pressure ≧ 250 mm Hg as an indication to stop testing but each institution will have to develop their own guidelines.
Example: The resting blood pressure was XXX/XX which is {within normal limits | elevated}. Blood pressure increased to XXX/XX during exercise which is {within normal limits | elevated}.
What was the systolic blood pressure 3 minutes post-exercise?
Blood pressure should be measured at 3 minutes following exercise termination. A (3 minute post-exercise systolic blood pressure / peak exercise systolic blood pressure) ratio greater than 0.95 indicates a blunted post-exercise decrease in blood pressure which is an indicator for an increased mortality risk.
Example: There was a {normal | blunted } decrease in systolic blood pressure following exercise.
What was the VO2 at Anaerobic Threshold?
A low VO2 at AT indicates an abnormal cardiovascular limitation (specifically a reduced O2 delivery to the exercising tissues). The LLN threshold (in terms of percent of the predicted VO2) rises with age:
Males:
- Age: 20 LLN: 42%
- Age: 30 LLN: 43%
- Age: 40 LLN: 44%
- Age: 50 LLN: 45%
- Age: 60 LLN: 46%
- Age: 70 LLN: 47%
Females:
- Age: 20 LLN: 41%
- Age: 30 LLN: 44%
- Age: 40 LLN: 47%
- Age: 50 LLN: 49%
- Age: 60 LLN: 52%
- Age: 70 LLN: 54%
Note: The Anaerobic Threshold generated automatically by test system software should always be verified. Determining Anaerobic Threshold is discussed in greater detail in the previous posting There’s more than one way to determine AT.
Example: The VO2 at Anaerobic Threshold was XX% of predicted which is {within normal limits | reduced}.
What was the Heart Rate – VO2 pattern?
The Heart rate and VO2 should be plotted against each other in a graph. Normally when this is done there should be a nearly straight line as the relationship between heart rate and VO2 tends to be linear. An upwards inflection in this line indicates that the heart rate is increasing faster than the VO2 and is an indication of a rate-related decrease in stroke volume which is often seen in valvular disease.
Note: This is discussed in greater detail in the previous posting Chronotropic Index and O2 Pulse.
Example: {There was a normal Heart-Rate VO2 pattern} | {There was an abnormal upwards inflection in the Heart Rate-VO2 curve occurring at a heart rate of XXX BPM.}
What was the O2 pulse pattern?
O2 Pulse is VO2/Heart rate (ml of oxygen consumed per heart beat). A normal O2 Pulse response pattern shows an immediate upswing at the beginning of exercise and a steady increase thereafter with a peak at peak exercise. An early plateau can be abnormal. An O2 Pulse that increases and then decreases is definitely abnormal and is usually seen in conjunction with an abnormal HR/VO2 curve.
O2 Pulse is the product of the a-v O2 Content difference and Stroke Volume. If there is no desaturation during exercise then O2 Pulse can be an indicator of Stroke Volume.
O2 Pulse usually decreases when exercise stops. An increase in O2 Pulse after the end of exercise is abnormal an usually seen in left ventricular dysfunction and other heart diseases.
Note: This is discussed in greater detail in the previous posting Chronotropic Index and O2 Pulse.
Example: {The O2 pulse pattern was normal.} | {There was an abnormal decrease in O2 pulse during exercise} | {There was an abnormal increase in O2 pulse following exercise.}
What was the maximum O2 pulse?
The maximum predicted O2 pulse is calculated from:
(Predicted Maximum VO2 (ml) / Predicted Maximum Heart Rate)
A maximum O2 pulse < 80% of predicted is likely abnormal and can indicate a stroke volume limitation or an inadequate exercise test effort.
Example: The maximum O2 pulse was XX.X ml/beat which is {within normal limits | reduced}.
The circulatory response to exercise primarily involves the delivery of oxygen to the exercising muscles. After having gone through this checklist it should be apparent whether the circulatory response to exercise was normal or abnormal, and as importantly, specifically which element was normal or abnormal.
A significant reduction in cardiac output is primarilysignaled by a reduced VO2 at AT and is usually due to either a decrease in stroke volume or the inability to increase heart rate (chronotropic incompetence). Depending on its severity a reduction in stroke volume is usually indicated by a reduced maximum O2 pulse while chronotropic incompetence is usually indicated by a reduced Chronotropic Index. These findings are not mutually exclusive, however and some patients will have both indications.
It should also be apparent that it is necessary to review all of the raw test data, not just that presented for baseline, AT and peak exercise. Summary reports automatically generated by test systems often have inaccuracies in how test data is selected and averaged and these reported results should always be verified.
Previous: Interpreting CPET Tests, part 2: Gas Exchange
Next: Interpreting CPET Tests, part 4: Interpretation and Summary
References:
Wasserman K, Hansen JE, Sue DY, Stringer WW, Whipp BJ. Principles of exercise testing and interpretation, 4th edition. Lippincott, Williams and Wilkins, publisher.

PFT
Blog by Richard
Johnston
is
licensed under a Creative
Commons Attribution-NonCommercial 4.0 International License.

Hi, Richard. How do you rate CMI in patients with atrial fibrillation?
Andrey –
I assume you’re talking about the Chronotropic Index or at least something like that. The simple answer is that cardiac output is dominated by ventricular contractions, not atrial so in general I use the ventricular rate in cardiac calculations. Atrial fibrillation can affect ventricular filling however, and for this reason may be a factor in a cardiac limitation to exercise, which is usually shown by a reduced VO2 at Anaerobic Threshold.
Regards, Richard
*Chronotropic Metabolic Index = chronotropic index