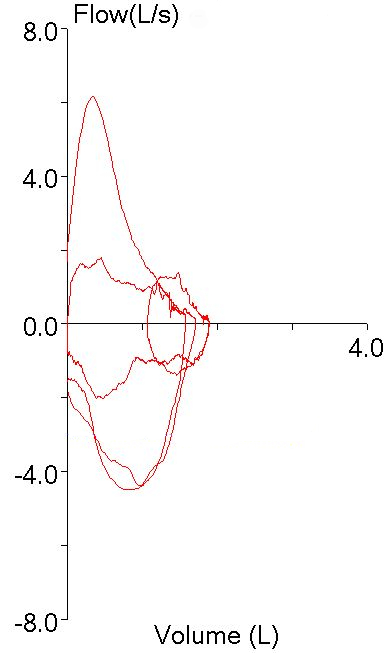
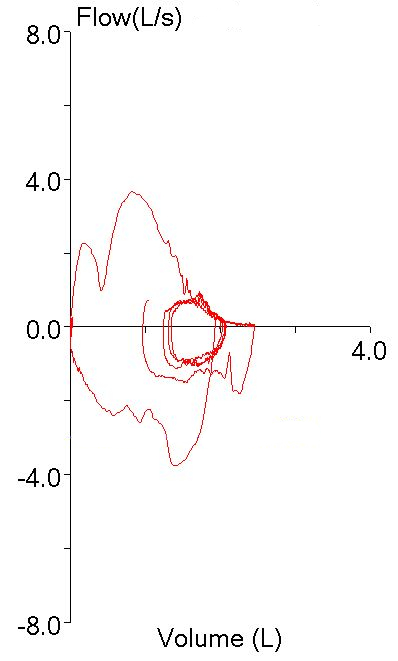
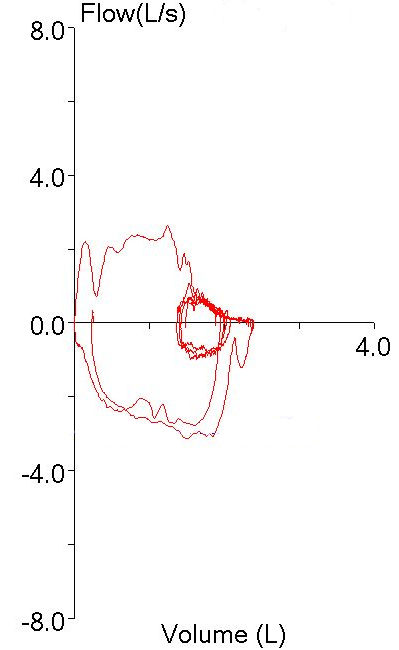
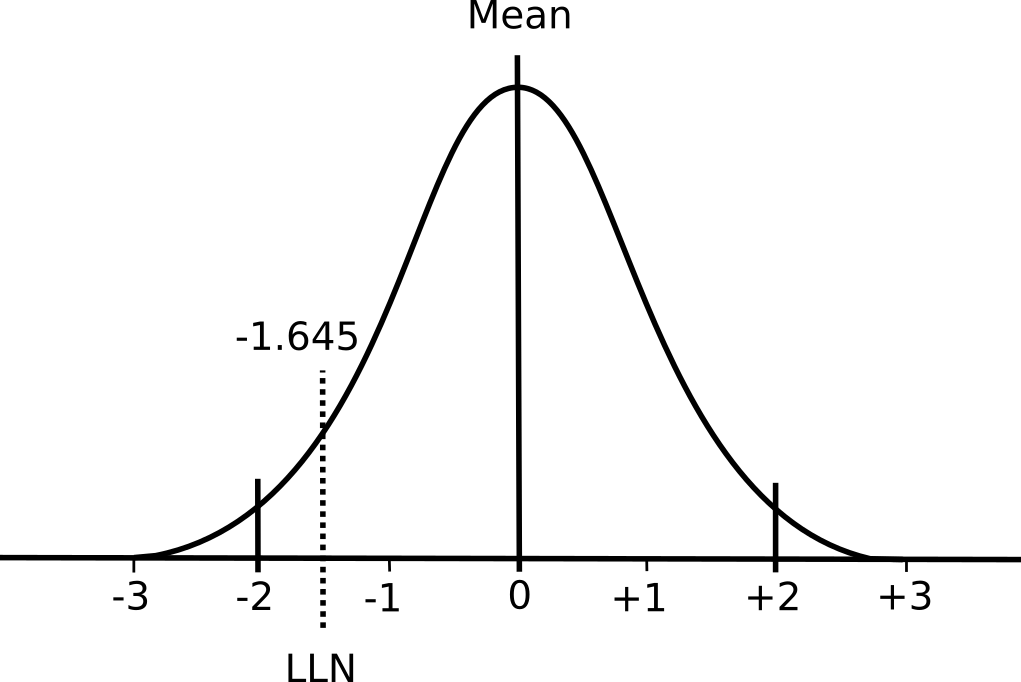
A couple weeks ago I was asked whether it was safe for a patient with an abdominal aortic aneurysm (AAA) to have pulmonary function testing. My first thought was that it was probably unsafe but after a moment or two of thought I realized that I hadn’t reviewed the subject for a long time. When I checked the 2005 ATS/ERS general testing guidelines (there are no contraindications in the 2005 spirometry guidelines) I found that AAA wasn’t mentioned at all. In fact, the only absolute contraindication mentioned was that patients with a recent myocardial infarction (<1 month) should not be tested. Some relative contraindications were mentioned:
- chest or abdominal pain
- oral or facial pain
- stress incontinence
- dementia or confusional state
and activities that should be avoided prior to testing include:
- smoking within 1 hour of testing
- consuming alcohol within 4 hours of testing
- performing vigorous exercise within 30 minutes of testing
- wearing clothing that restricts the chest or abdomen
- eating a large meal with 2 hours of testing
but these were factors where test results were likely to be suboptimal and not actually contraindications.
This got me curious since I thought that pulmonary function testing was contraindicated for more conditions than just an MI. I reviewed the 1994 and and then the 1987 ATS statements on spirometry but again found no mention of contraindications. Ditto on the 1993 ERS statement on spirometry and lung volumes. Finally, in the 1996 AARC clinical guidelines for spirometry I found a much longer list of contraindications:
- hemoptysis of unknown origin
- pneumothorax
- recent mycardial infarction
- recent pulmonary embolus
- thoracic, abdominal or cerebral aneuysms
- recent eye surgery
- presence of an acute disease process that might interfere with test performance (e.g. nausea, vomiting)
- recent surgery of thorax or abdomen
So where did the AARC’s list of contraindications come from? And why is there such a discrepancy between the ATS/ERS and the AARC guidelines?
Continue reading →