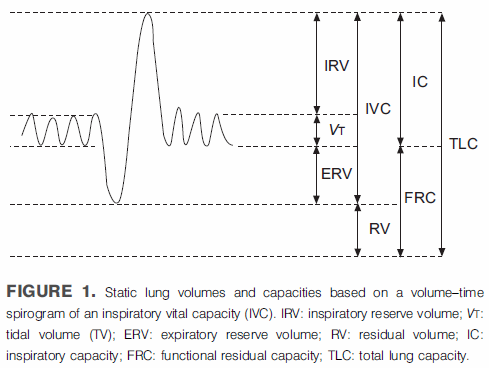
I had mentioned previously that my PFT Lab has been questioned why the percent predicted Residual Volume (RV) measurements on some research patients were coming out so much lower at my lab than at some other PFT Labs. At that time the researchers had not shared the results they had from these patients so we could only speculate that either our RV’s were actually lower or that the predicted RV values used by the other PFT Labs were different than ours. We finally got a copy of the PFT report for one of these patients and it turns out that both answers were correct.
First, the predicted RV from what I will call Lab X (I am not familiar with the lab nor with any of the physicians or technicians there) was 15% lower than ours. My lab is using the reference equations from Stocks et al which are recommended by the ERS. I was unable to determine which sets of reference equations Lab X was using. They weren’t listed on the report and the calculated values didn’t seem to match any of the reference equations I have on hand. Our lab software uses the predicted RV plus the predicted Forced Vital Capacity (FVC) (from NHANESIII) to calculate predicted Total Lung Capacity (TLC). It is possible that Lab X’s software calculates the predicted RV by subtracting their predicted FVC from a predicted TLC.
I am not, however, going to try to argue that my lab’s predicted values are better than those of Lab X, just that they are different. The ATS has not officially recommended any particular set of lung volume reference equations and I think it would be easy to argue that all current reference equations are flawed to one extent or another. I would like to know how they were derived at Lab X but that is just to satisfy my own curiosity. Using Lab X’s predicted RV, our measured RV was 179% of predicted where by our reference equations it was 152% of predicted. This explains part of the difference in percent predicted values but by no means all of it.
When I looked at the actual test results from Lab X however, I saw numerous errors in the lung volume test and test calculations.
Continue reading →