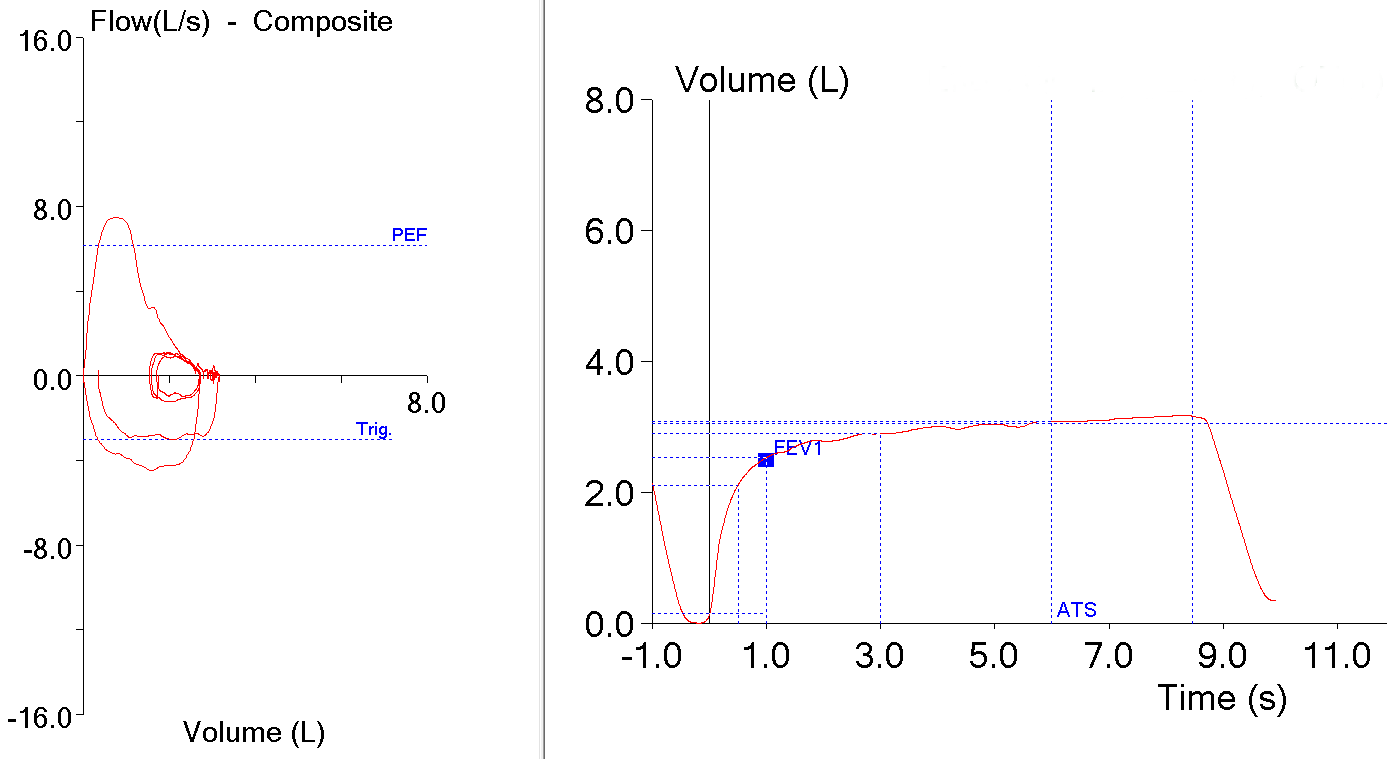
The single-breath DLCO maneuver can rightly be criticized as being an artificial maneuver that bears little resemblance to normal breathing. It is only by standardizing the maneuver that clinically relevant and reproducible results can be obtained. One important aspect of this standardization is the breath-holding period.
The single-breath DLCO maneuver begins with a subject exhaling to RV, followed by an inhalation of the test gas mixture to TLC and then a 10-second breath-holding period, ending with an exhalation during which a sample of alveolar air is collected. The initial choice of a 10-second breath-hold period was largely arbitrary and was selected in order to strike a balance between being a short enough period that for most patients to hold their breath, long enough to minimize the inspiratory and expiratory phases and long enough to allow for a sufficiently measurable amount of carbon monoxide to be taken up.
During the inspiratory phase of the DLCO maneuver, carbon monoxide uptake does not begin until the inhaled gas has passed both the test system’s and the subject’s anatomic dead space and reached the first functional alveolar-capillary unit. The full rate of carbon monoxide uptake will not occur until the diffusing gas mixture has reached all available alveolar-capillary units and these units have reached their maximum surface area. The rate of carbon monoxide uptake therefore increases throughout inhalation and reaches a maximum near TLC.
During the exhalation phase, carbon monoxide uptake continues even as the alveolar sample is being taken. For this reason the concentration of carbon monoxide at the beginning of the sampling period tends to be higher than at the end of the sampling period. The size of the washout volume and the alveolar sample volume, which to some extent determines how long a patient has to exhale before the acquisition of an alveolar sample is complete, will also have an effect on exhaled gas concentrations.
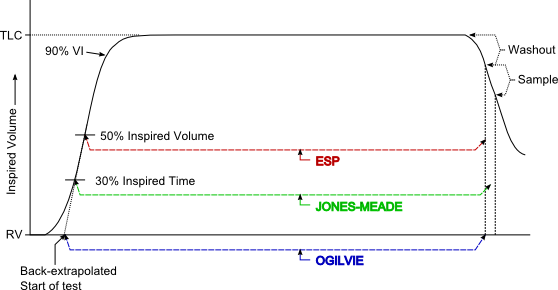
Because the point at which carbon monoxide uptake starts and the point at which it ends are to some degree indeterminate, several methods for standardizing the measurement of the single-breath DLCO breath-hold period have been developed. Of these, the Ogilvie method starts measuring the breath-hold period at the very beginning of inhalation and stops at the beginning of the alveolar sampling period. The Epidemiology Standardization Project (ESP) method, on the other hand, also stops at the beginning of the alveolar sampling period but instead starts measuring at 50 percent of the inhaled volume. Finally, the Jones-Meade method starts measuring at 30 percent of the inspiratory time and stops in the middle of the alveolar sampling period.
Continue reading →