The static respiratory pressures, Maximal Inspiratory Pressure (MIP or PIMAX) and Maximal Expiratory Pressure (MEP or PEMAX) are a way to non-invasively assess respiratory muscle strength. Respiratory muscle weakness is present in a number of conditions, most notably neuromuscular diseases and disorders, but also malnutrition, cardiovascular disease, polymyositis, sarcoid and COPD. Strictly speaking, the maximal inspiratory and expiratory pressures are not generated solely by the respiratory muscles but also by the elastic recoil. The elastic recoil of the lung at TLC contributes up to 40 cm H2O towards MEP and the elastic recoil of the chest wall at RV contributes up to 30 cm H2O towards MIP. Even so, an individual cannot reach TLC or RV without the use of their respiratory muscles so the measurements are still valid regardless of how the pressures are generated.
I have mixed feeling about MIPs and MEPs but this is mostly because many patients perform these tests poorly, making it hard to interpret results. Normal results can rule out respiratory muscle weakness but reduced results are not necessarily diagnostic. Nevertheless, they are still valuable tests and it is important for them to be performed correctly.
MIP is measured at RV and MEP is measured at TLC. The ATS/ERS statement on respiratory muscle testing indicates that each effort should last at least 1.5 seconds and that at least three measurements within 20% of the highest value should be obtained. A maximum number of attempts has not been specified but most research studies limited this to 5 or 6.
The actual maneuver depends somewhat on the equipment configuration. Respiratory pressures were originally measured using a pressure gauge and most early systems consisted of just a mouthpiece and a gauge (or gauges).

from ‘Interpretation of Pulmonary Function Tests – A Practical Guide’ by RE Hyatt, PD Scanlon and M Nakamura, Published by Lipincott-Raven, 1997, page 90.
To use this type of system the patient either exhales to RV or inhales to TLC, places their lips around the mouthpiece and then forcefully inhales or exhales. Because of the limited amount of time available for lip placement a round plastic or cardboard mouthpiece is usually used.
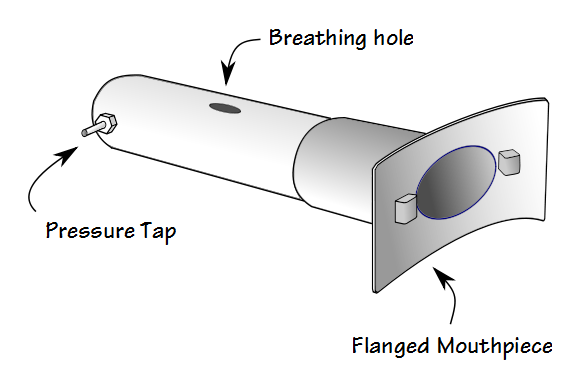
Currently, most MIP-MEP mouthpiece manifolds have a side hole that the patient can breathe through prior to performing a MIP or MEP maneuver.
This allows the use of a flanged mouthpiece which usually takes longer to insert and seat properly inside a patient’s mouth. With these types of manifolds the patient is placed on the mouthpiece first and allowed to breath normally until they are instructed to exhale to RV or inhale to TLC. The technician then blocks the hole and the patient then forcefully inhales or exhales. After the measurement the technician unblocks the hole and allows the patient to return to normal breathing.
Regardless of what type of a mouthpiece system is used a small leak must be built into it. This is intended to prevent glottal closure and the use of cheek muscles. The ATS/ERS statement specifies a hole with a 2 mm internal diameter that is 20-30 mm long (the length gives the leak a controlled resistance).
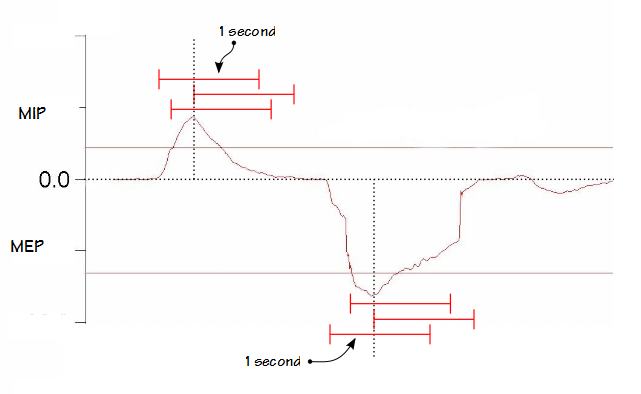
Although a side-hole manifold can be used with a pressure gauge the ATS/ERS standard makes the use of an electronic pressure transducer more or less mandatory. There are a couple reasons for this. First, reading pressure off a gauge during the relatively short time a patient inhaling or exhaling can be difficult. Although there are recording gauges (a secondary needle that is moved by the primary needle and remains at the highest pressure until reset) what is most likely to be reported is the peak pressure and that is not necessarily what is supposed to be recorded. Instead of the peak pressure (which could be a spike lasting only a short time), the ATS/ERS standards state that the maximum pressure should be averaged over a 1 second period and this is not possible with a gauge. Averaging requires an electronic pressure transducer and a computer with software designed to analyze the pressure signal and perform the averaging.
I have been unable to find any study that looked at the difference between peak and averaged MIP and MEP measurements. Since the point of the MIP and MEP tests are to measure respiratory muscle strength averaging is probably the best way to reject transient pressure spikes. The 1 second averaging period is relatively arbitrary and some studies have used different averaging periods, but since the averaging of MIP and MEP waveforms has not been studied in detail its not clear if there is an optimum averaging period.
More importantly though, the ATS/ERS statement only specifies that a 1-second average should be computed, not how it should be computed. This leaves it to individual researchers and manufacturers to decide how to implement an averaging algorithm. Presumably the peak MIP or MEP is used to select the proper segment of data for an averaging algorithm, but its not clear how much data before or after the peak pressure should be averaged. When I review the MIP and MEP results from our test systems it is unclear what part of the pressure waveform is being averaged (or should be averaged for that matter).
It also depends on how an algorithm is written whether a short effort (<1 second; which is admittedly a suboptimal effort but may also be the best the patient can do) will be underestimated or not. This may or may not make a significant difference in the reported MIP or MEP but it should be addressed the next time the ATS/ERS updates their standards.
Interestingly, several studies have shown that patients tend to get higher MIP and MEP pressures with a simple round mouthpiece than with a flanged mouthpiece. The reasons for this are unclear but the ATS/ERS statement nevertheless recommends a flanged mouthpiece which is because “These mouthpieces are also easier for patients to use, especially those with neuromuscular disease.”
So once you’ve gotten good quality MIP and MEP measurements, what’s normal?
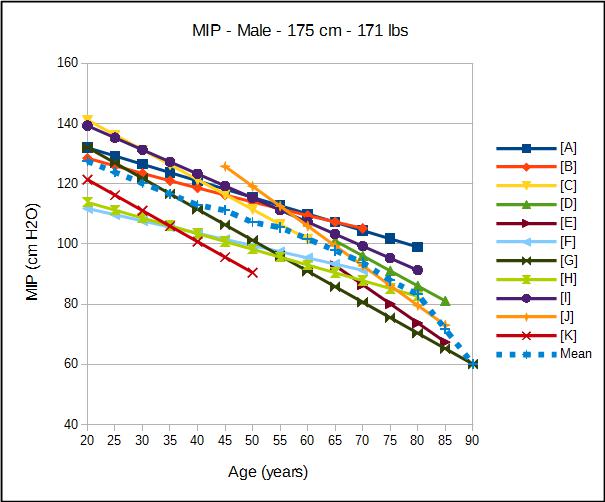
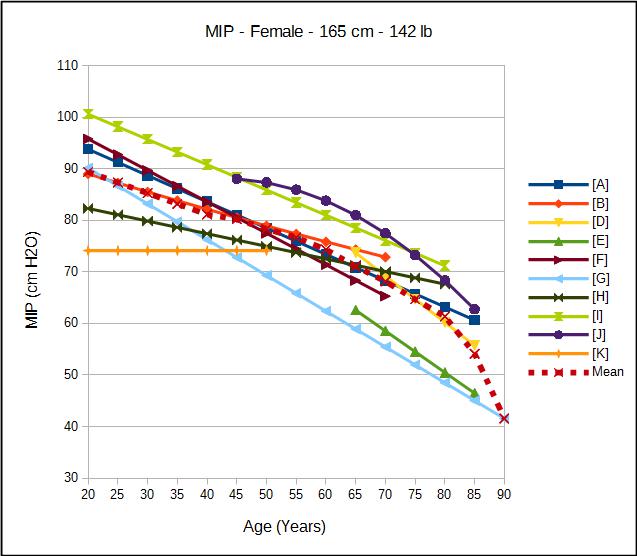
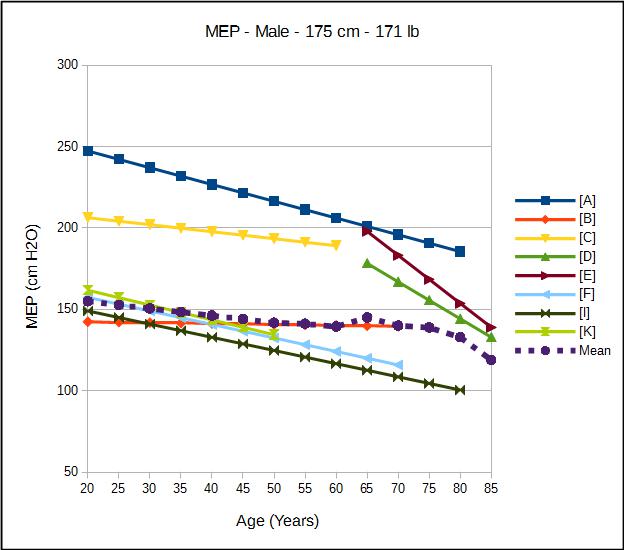
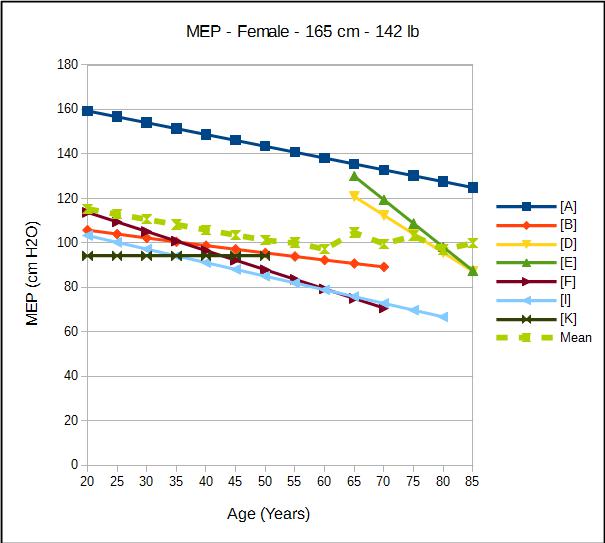
The predicted values for both MIP and MEP decrease with age and are larger for males than for females. Interestingly, height and ethnicity are not significant factors in most or all MIP and MEP reference equations. Unlike most other pulmonary function tests weight in one form or another (i.e. BSA or BMI) is a significant factor in most MIP and MEP reference equations. Not surprisingly, increased weight increases the predicted MEP in most instances. Somewhat surprisingly however, increasing weight also usually increases the predicted MIP. The reason for this relationship was not generally discussed except for one researcher who attributed it to an increased diaphragmatic strength.
As with many pulmonary function tests the normal values for MIP and MEP are spread over a relatively large range, and as usual selecting a single set of reference equations is problematic. The studies with the largest populations are limited to older individuals (45-85) and the studies with the widest age ranges were performed on relatively small populations. Because it’s particularly difficult to make a nuanced interpretation of MIP and MEP (basically all you can say is normal or abnormal) in this particular instance I’d recommend looking at the lower limit of normal instead.
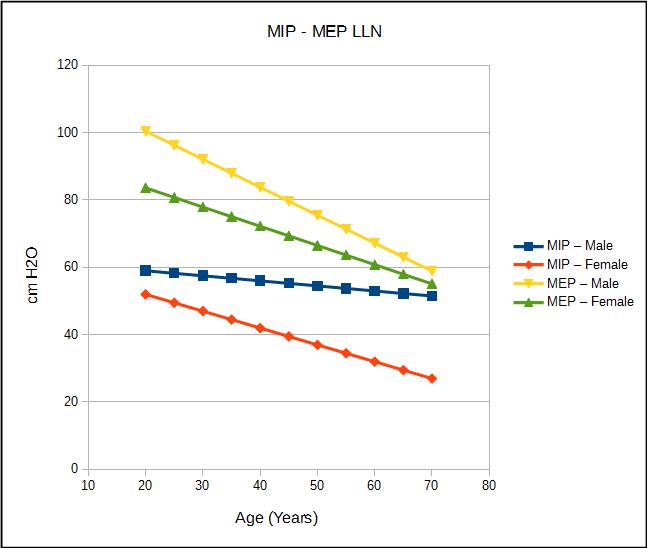
The ATS/ERS standard states that a “PIMAX of -80 cm H2O usually excludes clinically important inspiratory muscle weakness”. This statement isn’t referenced to any study however, and is not necessarily supported by research data. Evans et al performed an extensive analysis of the LLN for MIP and MEP and developed several reference equations which seem pretty reasonable.
| Male: | Female: | |
| MIP LLN: | 62 – (0.15 x age) | 62 – (0.50 x age) |
| MEP LLN: | 117 – (0.83 x age) | 95 – (0.57 x age) |
MIP and MEP are useful tests for assessing respiratory muscle strength that can be performed with relatively simple equipment. They are particularly useful for monitoring patients with known neuromuscular diseases and disorders. They should also be performed when patients with otherwise normal pulmonary function tests continue to complain of dyspnea and exercise intolerance.
MIP and MEP are very effort-dependent test and more than one study has indicated that a properly trained technician can make a significant difference in a patient’s test results. Patients need to be encouraged properly and particularly since these tests are frequently ordered for patients with neuromuscular diseases their lips and mouth needs to be checked during the test for a proper seal. For those patients that are unable to maintain a tight seal it may be possible to substitute a mask. Mask and mouthpiece MIPs and MEPs have been studied in normal subjects and although mask pressures were less than those obtained by mouthpiece the difference was not statistically significant.
MIP and MEP testing requires only relatively simple and inexpensive equipment. Many lab testing systems come equipped to perform MIP and MEP testing without the need to order it as an additional option. There is no CPT4 code for MIP and MEP testing however, (we use 94799, unlisted service) and some insurance companies will not pay for testing. I’ve read that some PFT labs don’t perform MIPs and MEPs for this reason but there are several tests we routinely perform (supine spirometry, for example) that we aren’t fully reimbursed for. I think this is just part of taking care of our patients, but the decision to offer or not to offer specific tests is sometimes made by hospital administration, not the lab.
| Male: | MIP Reference Equations: |
| Source: | Equation: |
| [A] | 143 – (0.55 x age) |
| [B] | 2.71828183^(4.02 – (0.004 x age) + (0.47 x BSA)) |
| [C] | 161 – (0.99 x age) |
| [D] | 149 – age + (0.1 x wt_lb) |
| [G] | 126-(1.028 x age) + (0.343 x wt_kg) |
| [H] | 10.2 x (0.158 x BMI) – (0.051 x age) + 8.22) |
| [I] | 155.3 – (0.80 x age) |
| [J] | 9.8-(0.31 x age)+(1.47 x wt_lb) – (0.0026 x (wt_lb^2)) – (0.0059 x age x wt_lb) |
| [K] | 142 – (1.03 x age) |
| Female: | MIP Reference Equations: |
| Source: | Equation: |
| [A] | 104 – (0.51 x age) |
| [B] | 2.71828183^(3.76 – (0.004 x age) + (0.47 x BSA)) |
| [D] | 118 – (0.9 x age) + (0.1 x wt_lb) |
| [G] | 171 – (0694 x age) + (0.861 x wt_kg) – (0.743 x ht_cm) |
| [H] | 10.2 x (8.55 – (0.24 x age)) |
| [I] | 110.4 – (0.49 x age) |
| [J] | -388+(1.77 x age)-(0.014 x (age^2))+(wt_lb x 0.41)-(0.0041 x age x wt_lb)+(4.69 x ht_cm)-(0.014 x (ht_cm^2)) |
| [K] | (0.71 x ht_cm) – 43 |
| Male: | MEP Reference Equations: |
| Source: | Equation: |
| [A] | 268 – (1.03 x age) |
| [B] | 2.71828183^(4.48 – (0.0004 x age) + (0.25 x BSA)) |
| [C] | 215 – (0.43 x age) |
| [D] | 278 – (2.27 x age) + (0.28 x wt_lb) |
| [I] | 165.3 – (0.81 x age) |
| [K] | 180 – (0.91 x age) |
| Female: | MEP Reference Equations: |
| Source: | Equation: |
| [A] | 170 – (0.53 x age) |
| [B] | 2.71828183^(4.3 – (0.0004 x age) -(0.003 x age) + (0.25 x BSA)) |
| [D] | 179 – (1.68 x age) + (0.36 x wt_lb) |
| [I] | 115.6 – (0.61 x age) |
| [K] | 3.5 + (0.55 x ht_cm) |
MIP/MEP Study Populations:
| Source: | #male | age range | #female | Age Range: | Ethnicity: |
| [A] | 60 | 20-74 | 60 | 20-74 | Not specified |
| [B] | 266 | 18-70 | 359 | 18-70 | Not specified |
| [C] | 101 | 20-59 | Caucasian | ||
| [D] | 112 | 65-85 | 176 | 65-85 | Not specified |
| [E] MEP | 329 | 65-85 | 427 | 65-85 | 96% Caucasian, 4% Black |
| [E] MIP | 2259 | 65-85 | 2942 | 65-85 | 96% Caucasian, 4% Black |
| [F] | n/a | n/a | Synthesized from other studies | ||
| [G] | 139 | 20-90 | 128 | 20-90 | Not specified |
| [H] | 248 | 18-82 | 256 | 18-82 | Not specified |
| [I] | 50 | 20-80 | 50 | 20-80 | Brazilian |
| [J] | 1886 | 45-84 | 1963 | 45-84 | White, Black, Asian, Hispanic |
| [K] | 48 | 18-50 | 87 | 18-50 | Caucasian |
MIP/MEP Study Methods:
| Source: | Year: | Measured By: | Mouthpiece | Sample: |
| [A] | 1969 | Gauge | Rubber, round | Peak |
| [B] | 1992 | Transducer | Plastic, oval | Peak |
| [C] | 1987 | Transducer | Plastic, round | Peak |
| [D] | 1995 | Transducer | Cardboard, round | Peak |
| [E] MEP | 1994 | Gauge | Rubber, flanged | 0.5 sec averaged |
| [E] MIP | 1994 | Gauge | Plastic, round | 0.5 sec averaged |
| [F] | 2009 | n/a | n/a | n/a |
| [G] | 1998 | Transducer | Cardboard, round | 2 sec Plateau |
| [H] | 2000 | Transducer | Rubber, round | 2 sec Plateau |
| [I] | 1999 | Guage | Plastic, flanged | 1 sec |
| [J] | 2009 | Gauge | Cardboard, round | Visually averaged, rounded to nearest 5 cmH2O |
| [K] | 1984 | Gauge | Plastic, flanged | 1 sec, Peak |
References:
ATS/ERS Statement on respiratory muscle testing. Am J Respir Crit Care Med 2002; 166: 518-624.
[A] Black LF, Hyatt RE. Maximal respiratory pressures: normal values and relationship to age and sex. Am Rev Respir Dis 1969; 99: 696-702.
[B] Bruschi C, Serveri I, Zoia MC, Fanfulla F, Fiorentini M, Casali L, Grassi M, Grassi C. Reference values of maximal respiratory mouth pressures: A population-based study. Am Rev Respir Dis 1992; 146: 760-793.
[C] Cordain L, Glisan BJ, Latin RW, Tucker A, Stager JM. Maximal respiratory pressures and pulmonary function in male runners. Brit J Sports Med 1987; 21(2): 18-22.
[D] Enright PL, Adams AB, Boyle PJ, Sherill DL. Spirometry and maximal respiratory pressure references from health Minnesota 65 to 85-year-old women and men. Chest 1995; 108: 663-669.
[E] Enright PL, Kronmal RA, Manolio TA, Schenker MB, Hyatt RE. Respiratory muscle strength in the elderly. Correlates and reference values. Am J Respir Crit Care Med 1994; 149: 430-438.
[F] Evans JA, Whitelaw WA. The assessment of maximual respiratory mouth pressure in adults. Respir Care 2009; 54(10): 1348-1359.
[G] Harik-Khan RI, Wise RA, Fozard JL. Determinants of maximal inspiratory pressure. Am J Respir Crit Care Med 1998; 158: 1459-1464.
[H] Hautmann H, Hefele S, Schotten K, Huber RM. Maximal inspiratory mouth pressures (PIMAX) in healthy subjects – what is the lower limit of normal? Respir Med 2000; 94: 689-693.
McElvaney G, Blackie S, Morrison NJ, Wilcox PG, Fairbarn MS, Pardy RL. Maximal static respiratory pressures in the normal elderly. Am Rev Respir Dis 1989; 139: 277-281.
[I] Neder JA, Andreoni S, Lerario MC, Nery LE. Reference values for lung function tests: II. Maximal respiratory pressures and voluntary ventilation. Braz J Med Biol Research 1999; 32: 719-727.
[J] Sachs MC, Enright PL, Hinckley Stukovsky KD, Jiang R, Barr RG. Performance of maximum inspiratory pressure tests and maximum inspiratory pressure reference equations for 4 race/ethnic groups. Respir Care 2009; 54(10): 1321-1328.
[K] Wilson SH, Cooke NT, Edwards RHT, Spiro SG. Predicted normal values for maximal respiratory pressures in caucasian adults and children. Thorax 1984; 39: 535-538.
Wohlgemuth M, van der Kooi EL, Hendriks JC, Padberg GW, Folgering HT. Face mask spirometry and respiratory pressures in normal subjects. Eur Respir J 2003; 22: 1001-1006.

PFT Blog by Richard Johnston is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License

Thanks, Richard.
I’m wondering if, on a combined “Spirometry- Lung Volumes- Single Breath Diffusion- MIP/MEP” report form, where all tests were given and results entered (except for the MIP/MEP test, which is left blank), would a blank MIP/MEP entry on the form be because: the patient’s TLC and RV lung volume values were normal, and therefore the MIP/MEP test wasn’t necessary?
I other words, if the reason the MIP/MEP test wasn’t given as a routine matter (because of lack of insurance coverage reimbursement), the dept. (I’m guessing) would leave the MIP/MEP test entry off the form altogether.
Ed
Ed –
TLC and RV don’t have all that much to do with MIP and MEP unless MIP and MEP are severely reduced. The reason is probably far more prosaic. Every report format must be created and maintained. My lab has about a dozen report formats but they don’t cover all of the possible combinations of tests we could perform. That would need somewhere around 40-50 different formats. If you need to make some kind of change in what you are reporting that means you have to make the same change on each and every report format it applies to (!!!) which, needless to say is a pain. It is easier use a relatively general report format and know that some of the reported information will be blank than to try to have report formats for all possible situations. Equipment manufacturers put only minimal effort into their report generators and we’re stuck trying to use them as best we can.
– Richard
hola, te felicito por el blog, me podrias mandar el articulo de valores de corte de MIP , MEP de 30 y 40 cmh20 respectivamete. Gracias
(Google translation: Hello, I congratulate you on the blog, Could you send the article cutoff values of MIP, MEP 30 and 40 cm H20 respectively. thanks)
Rosalia –
It depends on the age and gender of the individual but realistically both the MIP and MEP are well below normal and would likely considered to be severely reduced.
(Google translation: Depende de la edad y el sexo del individuo, sino con realismo tanto en el MIP y el MEP son muy por debajo de lo normal y probablemente considerado ser severamente reducida.)
– Richard
Where do the high range manometers and manifolds come from?
Bill –
They’re not really available any more. The only dial gauge manometers I can find are used for bedside NIF’s on ventilator patients (for example see Tri-Anim) and they max out around 120 cm H2O. Nowadays the only full-range MIP-MEP meters (+/- 300 cm H2O) are electronic. For most PFT labs MIP-MEP measurements are part of full-range testing systems. The MicroRPM is the only handheld one I know and is sold by MDSpiro and Carefusion.
– Richard
Hi. Very interesting topic also…we asked this precise question in this large study (to be presented at ERS, 2016) which is under review in CHEST.
Title: Maximal inspiratory pressure: does the choice of reference values matter?
Mr. Antenor Rodrigues, Ms. Marianne Silva, , Prof. Dr Danilo Berton, Prof. Dr Denis O’Donnell and Prof. Dr J Alberto Neder, nederalb@gmail.com, MD. 1Department of Medicine, Division of Respirology, Queen’s University, Kingston, Ontario, Canada and 2Pulmonary Function Laboratory, Hotel Dieu Hospital, Kingston, Ontario, Canada.
Body: Background: Single-point measurements of maximal inspiratory pressure (MIP) are frequently used to suggest inspiratory muscle weakness. Although there is substantial disparity among predicted MIP according to specific regression equations, it remains unclear whether those discrepancies impact on the diagnosis of inspiratory muscle weakness in clinical practice. Methods: 1729 consecutive subjects (50.1% males, aged 18 to 94) who underwent MIP measurements in a reference laboratory. MIP was predicted according to the most cited MIP reference values. Diagnosis/suspicion of neuromuscular disease in a subject with restriction by body plethysmography indicated a “high” pre-test probability of weakness. Results: Prevalence of weakness ranged from 33.4 % (Enright et al.) to 66.9 % (Neder et al.). Black and Hyatt, Neder et al., and Bruschi et al. agreed well in indicating weakness (κ values ranging from 0.74 to 0.80; p<0.01) There was also significant agreement between pre-test probability of inspiratory muscle weakness and abnormally-reduced MIP according to those specific prediction equations (p<0.01). In contrast, a large fraction of patients presenting with “preserved” MIP according to Enright et al., Harik-Khan et al., Wilson et al. had a high pre-test likelihood of weakness. Absolute MIP values at which most equations agreed to indicate weakness in both genders were <60 cmH2O (< 40 yrs), <50 cmH2O (40-80 yrs) and 80 yrs). Conclusion: Prevalence of inspiratory muscle weakness is influenced by the reference values used for MIP prediction. Some specific regression equations are more closely related to clinical and physiological features suggestive of inspiratory muscle weakness than others.
Thanks, your article is very informative.
I’m a recently diagnosed MG patient who was in the ER with shortness of breath. The NIF test they did was with a peak reading gauge and I certainly didn’t try for more than a quarter to half-second. Is there a way to correlate that peak reading to a one second average?
Lee –
Nobody has attempted to correlate peak MIP (NIF) with an averaged one. Part of the reason is that the ATS/ERS statement is vague on how averaging should be performed so any correlation would depend highly on which averaging algorithm was used. When you say ‘gauge’ I’m assuming you mean a manometer. Many of the earlier studies on MIP and MEP (Black and Hyatt in particular) used this type of device. To some extent the fact that the gauge is mechanical (bourdon tube with gears) acts to level out the very short inspiratory or expiratory peaks and and any measured value shouldn’t be too far from an electronically averaged value.
Regards, Richard
Hi,
My MIP is 172 cmH2O despite never exercising and struggling to breathe all day every day.
What could this mean?
it has been suggested that there might be something attached to my diaphragm, pulling it down, preventing recoil and causing air packing. or something obstruction the diaphragm movement.
Any theories welcomed!
Bard –
MIP is pretty much a direct measurement of diaphragmatic muscle strength but adequate strength does not mean you will not have trouble with your breathing. Remember that the lung is meant to get O2 into the blood and CO2 out. The ability to ventilate the lung (i.e. a normal MIP) doesn’t mean the lung is working adequately otherwise.
– Richard