Yesterday while reviewing reports I ran across an interesting error in the Inspiratory Volume (VI) from a DLCO test. I’ve probably seen this before but this time I realized what effect it could have on DLCO. Specifically, what I saw was that at the start of the DLCO test the subject had not finished exhaling and although the technician had started the test, the subject continued to exhale.
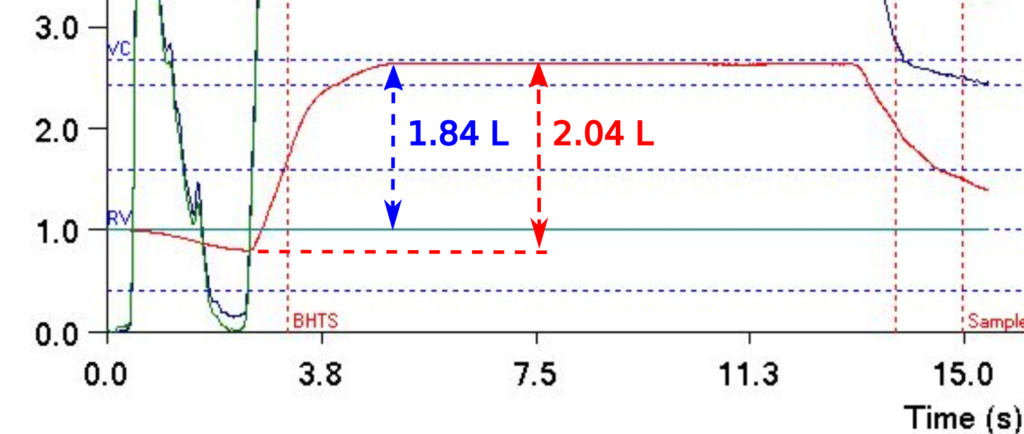
What makes this interesting is that the software used the subject’s volume at the start of the test as the initial volume. This means that the software measured the VI from the initial volume to the end of inspiration, not from the point at which the subject stopped exhaling to the end of inspiration. This also means that the VI was underestimated by 0.20 L and this affects both VA and the calculated DLCO.
VA is calculated by:
Where:
VA = alveolar volume (ml)
VI = inspired volume (ml)
Vd = machine + anatomical deadspace
Plugging in the original test values this is:
When the VI is adjusted for missing volume, it becomes:
which is a difference of 0.45 L and a 12% increase. As a reminder, the DLCO calculation formula is:
Given that BHT, Pb, PH20, FATrace, FiTrace, FICO and FACO are unchanged, then the increase in VA would in turn cause an increase in calculated DLCO of 12% as well.
For this particular subject, this error did not make a significant change in their reported DLCO since it increased from 50% of predicted to only 56% of predicted. For a subject that was at 75% of predicted however, the adjusted DLCO would have been 84% of predicted. By my lab’s criteria this would be a change from being mildly reduced to being within normal limits and that would have been a significant difference.
There is an opposite error in inspiratory volume that unfortunately we see more frequently than we’d like. Specifically, the expiratory valve in our test system’s manifolds often closes too slowly or leaks slightly and when this happens subjects often leak at the beginning of the breath-holding period.
The whole point of an adequate VI is to ensure the subject’s lungs are near TLC and at their maximum surface area during the breath-holding period. DLCO normally tends to decrease when the maximum inspiration is below 90% of TLC so an inadequate VI can cause DLCO to be underestimated. Interestingly however, even though most of the breath-holding period is at a lower lung volume which would normally result in a lower DLCO it will instead be higher than would be expected.
VA is a critical part of the DLCO calculation and as already noted is calculated from the VI and the ratio of the inhaled and exhaled tracer gas concentrations. To some extent the exhaled tracer gas concentration requires a certain amount of breath-holding time in order to be for it to be distributed homogeneously. The actual time needed for this to occur differs from subject to subject but individuals with normal lungs or restrictive disorders like Pulmonary Fibrosis will probably achieve a homogeneous concentration of tracer gas relatively quickly. For these subjects the reported VA will likely be whatever the lung volume was at the end of the initial inspiration.
For individuals with airway obstruction however, even the standard 10 seconds of breath-holding time is not sufficient for equilibration and when this occurs, the exhaled tracer gas concentration will probably be more in line with the lung volume that was present during most of the breath-holding period. For this reason, VA will still be overestimated due to the falsely elevated VI but not so much due to the dilution of the tracer gas.
Either way, VA will be overestimated but the subject actually spent most of their time at a lower lung volume. When breath-holding occurs at volumes below TLC, KCO (the rate at which CO disappears from the lung), tends to increase. This increase in KCO generally correlates with decreases in lung volume but not necessarily predictably or even linearly. Even so, given the combination of falsely elevated VA and a possible increase in KCO, DLCO will probably be overestimated in these circumstances.
So errors in test performance can cause the Inspiratory Volume to be under- or overestimated. Because of the relationship between VI and VA, and between VA and DLCO, an underestimated VI will cause DLCO to be underestimated and an overestimated VI will cause DLCO to be overestimated. This problem is exacerbated to some extent by the inability of our software to recognize any problems with the VI measurement in the first place and by that fact that our software doesn’t let us manually correct any of these errors.
Whether the Inspiratory Volume was underestimated or overestimated, it wouldn’t have been evident if I hadn’t taken a close look at the the volume graph from the DLCO test. I review the raw data for all DLCO tests performed in my lab so I routinely see these kinds of problems. Many reviewers however, only see the final report and either don’t or can’t see the raw test data. I’ve seen reports from dozens of labs around the United States and only a small number had a DLCO graph on the report and even then, it is almost always very small and any problems with the VI probably wouldn’t have been noticeable. The 2017 ERS/ATS DLCO standards mandates the presence of a DLCO graph on DLCO reports and if you’re going to implement this it makes sense to make sure it’s large enough for the details to be evident.
As importantly, although we report the VI along with the DLCO results, not all labs do. I think this is a mistake because it’s helpful in ensuring DLCO test quality to a reviewer. More than that though, since the ATS/ERS spirometry interpretation guidelines say that the FEV1/VC ratio is supposed use the largest VC from any test. Occasionally I find that the VI (which is an IVC) is larger than the FVC or SVC and knowing this can make a difference in the interpretation of spirometry results.

PFT Blog by Richard Johnston is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License

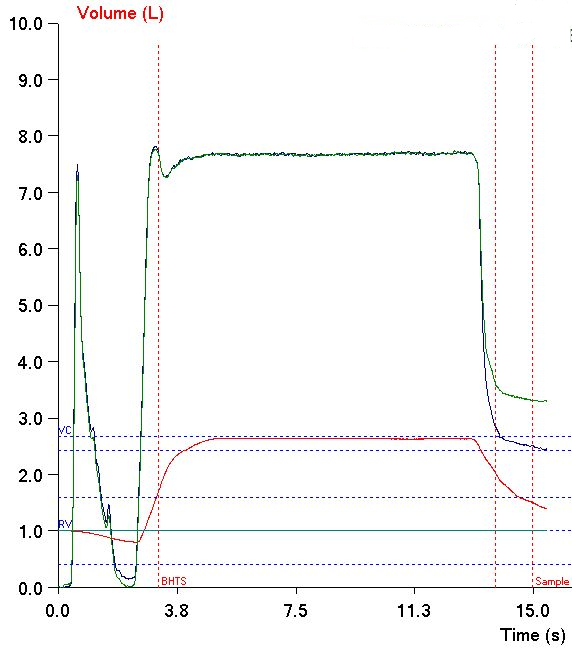

Richard, the last graph in your example seems to have an exhalation error if I am reading it correctly. The tracer gases seem to be released before the end of breath hold, the sample begins too soon, the sample volume looks too small and the dead space may not have been adequately cleared. Am I seeing this wrong?
I realize the example is for inspiration errors but is the automated programming messing up on exhalation. Thanks, David
David –
I agree, but it was the best example I could come up with on short notice and, as you said, I was interested in the inspiration and breath-holding volume, not the analyzer signals or the exhalation.
Regards, Richard
Dear Richard,
Nice to know you, and very interesting discussion in your blog. I’m looking forward for more interesting discussion and article. For me I’m working as respiratory technician and have 12 years experienced in doing LFT.
Thank you.
Richard,
Can you explain to me if there would ever be a time you would adjust the sample line, or better yet. where the computer chooses its sample from for the DLCO measurement. I don’t completely understand. We use the VMAX system and it seems at times the bar or line is not in places it should be and the results seem off.
Thank you.
Sarah –
I assume you’re talking about adjusting the washout and sample volumes that have been determined by the computer software? If so, then in all real-time DLCO systems part of the calibration process is to characterize the gas sample transport time from the breathing manifold to the gas analyzers and the 90% rise time of the gas analyzers. Theoretically, this process should allow the computer to accurately match the exhaled volume signal (integrated from expiratory flow) with the gas analyzer signals and therefore accurately determine the washout and sample volumes. That’s fine, except it doesn’t work all the time.
In my lab’s test systems I have noticed that when a patient exhales very rapidly the alveolar sample window tends to include some or much of the washout volume. When a patient exhales slowly, I find that the alveolar sample window tends to be placed well after the actual beginning of the alveolar plateau. For this reason I always review all DLCO tests performed in my lab and frequently find the need to adjust the alveolar sample window. The error isn’t usually all that large and usually doesn’t make a big difference in the reported DLCO, but at least once or twice a day it does make a significant difference and moves the DLCO from mildly reduced to normal, or something like that. I’ll also note that by doing this (i.e. adjusting the alveolar sample window) I also tend to see smaller visit-to-visit changes in DLCO.
To me this says that the matching of gas analyzer and expiratory volume signals doesn’t work as well as the manufacturer claims. It’s not clear to me where the error is coming (particularly since it is clearly related to the expiratory flow rate) from but I will note in passing that when we do back-to-back calibrations the transit time tends to differ by around 20-50 milliseconds (and sometimes more). That may not sound like much, but at an expiratory flow of 10 L/sec an error of only 10 milliseconds equates to 100 ml.
I will also note that the fact that there appears to be a certain level of mismatching between the expired volume and gas analyzer signals raises some concerns about the accuracy of the exhaled CO and CH4 values. These values should be averaged volumetrically which means that a certain gas concentration is applied to a certain volume. If volume and gas signals are mismatched however, that means the average CO and CH4 values may be distorted. Strictly speaking when the exhaled volume, CO and CH4 waveforms are flat any error is probably very tiny but when the volume waveform is curved and/or the CO and CH4 waveforms are sloping downwards, then there is the potential for a measurable error.
Anyway, I have absolutely no qualms about adjusting the alveolar sample window and you shouldn’t either.
Regards, Richard
Hello,
I’m fairly new to the PFT world and have a couple of questions.
First, regarding the inspiration tracing in the first example of this post: At the end of inspiration there’s a “peak” before the tracing levels off, it’s been suggested to me that this indicates a leak and would invalidate the results of this test. As I look at other examples, this doesn’t really look the same as other leaks I’ve noted…could someone explain to me what that is and if it effects test quality?
Second, is it common to use a valve closure/balloon inflation during the inspiratory hold? I work at two different facilities and one closes during inhalation, the other doesn’t unless the patient cannot hold their breath.
TIA for any thoughts or suggestions.
Debi
Debi –
I think it is the patient relaxing at a level below their true peak inhalation. Our test systems use a manual key stroke from the tech performing the test to lock the DLCO valve and they can be a bit slow to close the valve sometimes. The problem is that this maximal inhalation is used to calculate VA and the calculated DLCO scales with VA. If VA is significantly overestimated then DLCO will be overestimated.
– Richard