Recently I was trying to explain the effect of altitude on blood oxygenation to somebody with IPF. They had observed that their oxygen saturation was fairly normal at sea level but that they needed to use their supplemental O2 when they went up to 2000 feet and didn’t understand why such a low altitude made that much of a difference. I don’t think I did very well with the explanation since at the time I was limited to only text and I much prefer pulling out diagrams and waving my hands in the air.
The place to start is with the alveolar air equation.
Where:
PAO2 = partial pressure of O2 in the alveoli
FiO2 = fractional concentration of O2
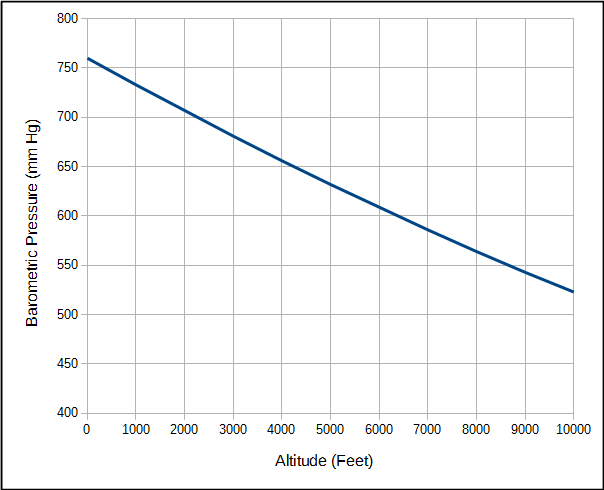
PB = barometric pressure
PH20 = partial pressure of water vapor in the alveoli
PaCO2 = partial pressure of CO2 in the arteries
RER = respiratory exchange ratio (VCO2/VO2)
When normal values are plugged into the alveolar air equation it looks like this:
An important point is that when air is inhaled into the lung oxygen is diluted by the water vapor and carbon dioxide that are already there. The partial pressure of oxygen will vary with atmospheric pressure but the partial pressure of water vapor and carbon dioxide are relatively fixed values. Atmospheric pressure of course decreases with altitude.