One of the key reasons to perform spirometry is to measure expiratory flow rates. The flow rate of air through any system is primarily a function of driving pressure and resistance. Since there are limits to anybody’s ability to increase driving pressure (and physiological reasons why airflow does not continue to increase when driving pressure exceeds a certain threshold value) FEV1 is largely related to the amount of resistance in the airways.
The gold standard for measuring airway resistance (Raw) has been plethysmography. Like many other pulmonary function tests measuring Raw depends on a series of assumptions and a standardized approach to assessing the results. One of the standardizations is that a Raw maneuver must always be paired with a TGV maneuver. Although the knowledge of lung volume allows values like specific resistance (sRaw) and specific conductance (sGaw) to be calculated, this is not the reason for the TGV maneuver at all.
Resistance is calculated from:
Inspiratory and expiratory flow rates are relatively easy to measure but the driving pressure, which in this case is alveolar pressure, is not. For this reason an indirect approach is needed to estimate alveolar pressure.
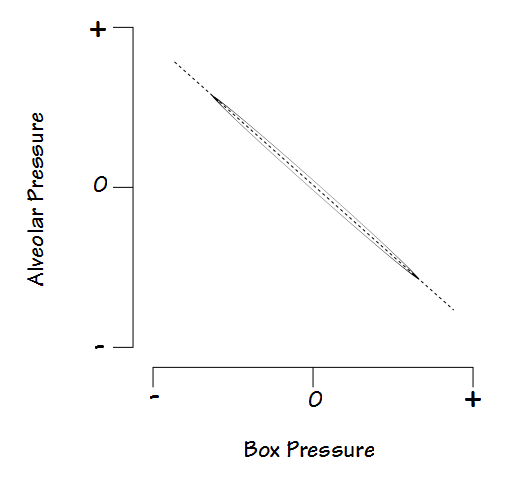
The measurement of lung volumes in a plethysmograph is made when a subject attempts to breathe against a closed mouthpiece. Pressure inside the mouthpiece (which is assumed to be alveolar pressure) is plotted against the pressure inside the box.
The slope of the line, which is
combined with knowledge of the volume of air inside the box and the scaling factors of the pressure signals allows thoracic gas volume (TGV, the volume in the lungs at the time the mouthpiece was closed) to be calculated. More importantly it also shows the relationship between alveolar pressure and box pressure.
The Raw test maneuver consists of having the subject pant through a flow sensor in a closed plethysmograph. Flow rate is plotted against box pressure.
Breathing requires a pressure gradient between the mouth and the alveoli. During inhalation pressure in the aveoli has to be less than the ambient atmospheric pressure and during exhalation is has to be greater. This means that when a subject breathes inside a closed plethysmograph because the volume of air inside the box does not change, box pressure will increase during inhalation and decrease during exhalation. Since the relationship between box pressure and alveolar pressure can be found from the TGV maneuver this means that alveolar pressure can be derived from box pressure.
The assumption that Palv is directly proportional to Pbox is not perfectly correct however. The airways are open to atmosphere during the Raw panting maneuver and closed off during the TGV maneuver. To correct for this it is usually assumed that the entire deadspace between the alveoli and mouthpiece (which includes the airways, mouth and apparatus deadspace) is on average at half the pressure of the alveoli. There is a somewhat complex formula that takes this into consideration but it is really the ratio between TGV and one-half the deadspace that matters and for most people this would indicate that Palv is probably underestimated by around 5%.
I have equivocal feelings about the clinical utility of Raw. About 20 years ago I was involved in performing Raw for a research study. The research subjects were highly motivated but we had to settle for a baseline repeatability of +/- 40% in Raw and SGaw even after multiple practice sessions and this made it hard to find any statistical significance in the study’s results (although strictly speaking there may not have been any significance but the researchers were convinced there was). This variability indicates that changes in Raw have to be large to be notable which is also reflected in the fact that the normal range for Raw is relatively large.
The contour of Raw loops can be diagnostic since different airway diseases can alter the loop in distinct ways. Recognition of flow-volume loop contours is aided by the fact that there is a standard convention for displaying flow and volume. This is not the case for Raw loops since I’ve found that which axis flow and box pressure are placed on as well as which direction is positive and which is negative can vary from one research article to another.
A final point is that the airway resistance during inspiration can be different from that during expiration particularly in lung diseases like emphysema. My lab’s test software does not allow us to make this differentiation and in fact averages the Raw slope from both inspiration and expiration.
The advantage of Raw measurements is that they can be performed near FRC. There are many researchers that believe that the deep inspiration that accompanies an FVC maneuver alters bronchial tone and affects the ability to recognize bronchoconstriction. In addition, it is possible for Raw maneuvers to be performed by individuals that are unable for any number of reasons to perform spirometry adequately.
Raw varies with lung volume in a curvilinear fashion and is lower at high lung volumes and higher at low lung volumes. Conductance (Gaw) which is the inverse of Raw (1/Raw) also varies with lung volume, but linearly. Specific conductance (SGaw) which is Gaw/TGV is reasonably linear across all lung volumes and it is for this reason that SGaw is probably the most useful and commonly reported value from Raw measurements. This is in itself a reason to perform a TGV maneuver along with a Raw maneuver, but without the TGV maneuver it wouldn’t be possible to measure Raw in the first place.
References:
Blonshine S, Goldman MD. Optimizing performance of respiratory airflow resistance measurements. Chest 2008; 134: 1304-1309.
Dubois AB, Botelho SY, Comroe JH. A new method for measuring airway resistance in man using a body plethysmograph: values in normal subjects and in patients with respiratory disease. J Clin Invest 1956; 35: 327-335.
Goldman MD, Smith HJ, Ulmer WT. Whole-body plethysmography. Eur Respir Mon 2005; 31: 15-43.
Hemingway A. Measurement of airway resistance with the body plethysmograph. Charles C. Thomas publisher, copyright 1973.
Kaminsky DA. What does airway resistance tell us about lung function? Respir Care 2012; 57(1): 85-96.

PFT Blog by Richard Johnston is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.


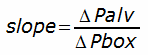

How high have you seen Raw be? I’ve been told that when the Raw is more than 250% of predicted value that the result is likely inaccurate. Assuming no thermal drift, panting frequency has been correct and that the technologist has corrected computer-generated tangents if necessary, how can one be sure that the Raw is accurate? If very high numbers are considered inaccurate, then what can be done to achieve better results?
Cindy –
I don’t have a good answer for you because my lab hasn’t done any clinical RAW measurements for over 20 years. None of the physicians we work with believe that RAW has any clinical value. To some extent I agree with this and that is because my personal experience is that it has poor reproducibility and the normal ranges are very broad. I will also admit to having some conceptual problems with SGAW and SRAW. I’ve performed RAW a fair amount for research but going in you have to accept a level of reproducibility (+/- 40% in the last study) that makes it hard to determine statistical significance. Moreover, our lab’s software is not able differentiate between inspiratory and expiratory airway resistance. Patients with COPD often have very broad, almost triangular-ish RAW traces and one edge is inspiratory and one is expiratory, yet the angles are very different. Our software insists on averaging this and although we can override it we then have to choose whether to report inspiratory or expiratory RAW.
Regards, Richard